Streamlining HIV testing in non-clinical settings
Using human-centered design to improve testing and reporting processes and enhancing public health response in underserved communities
Overview
Goals
Problem
We aimed to develop and implement an HIV reporting solution that empowers community-based organizations (CBOs) conducting testing to capture accurate data efficiently, enabling LAC’s health department to spend less time and effort on capturing data related to HIV diagnosis and more time and resources on increasing testing, especially among underserved populations. Long-term, we hope to scale the reporting solution nationwide and empower non-traditional and under-resourced testing facilities across the country to capture and report not just HIV, but other reportable conditions, seamlessly, enabling health departments to take necessary actions to protect their communities.
Since the emergence of the HIV epidemic, timely diagnosis and reporting have been vital to public health efforts. Undiagnosed cases are common, especially in underserved populations, due to challenges in testing and data reporting. To address this, our team partnered with clients in Los Angeles County and the CDC to streamline HIV testing and reporting in non-clinical settings, like community-based organizations (CBOs). These organizations often lack IT infrastructure, relying on paper records and faxing results—an inefficient, error-prone process that delays public health response and hampers timely interventions.
Role
Project / user research lead
tools
Figma
Respondent
Dovetail
Duration
6 months
Methods
Contextual inquiry
Interviews
Concept testing
Usability testing
My approach
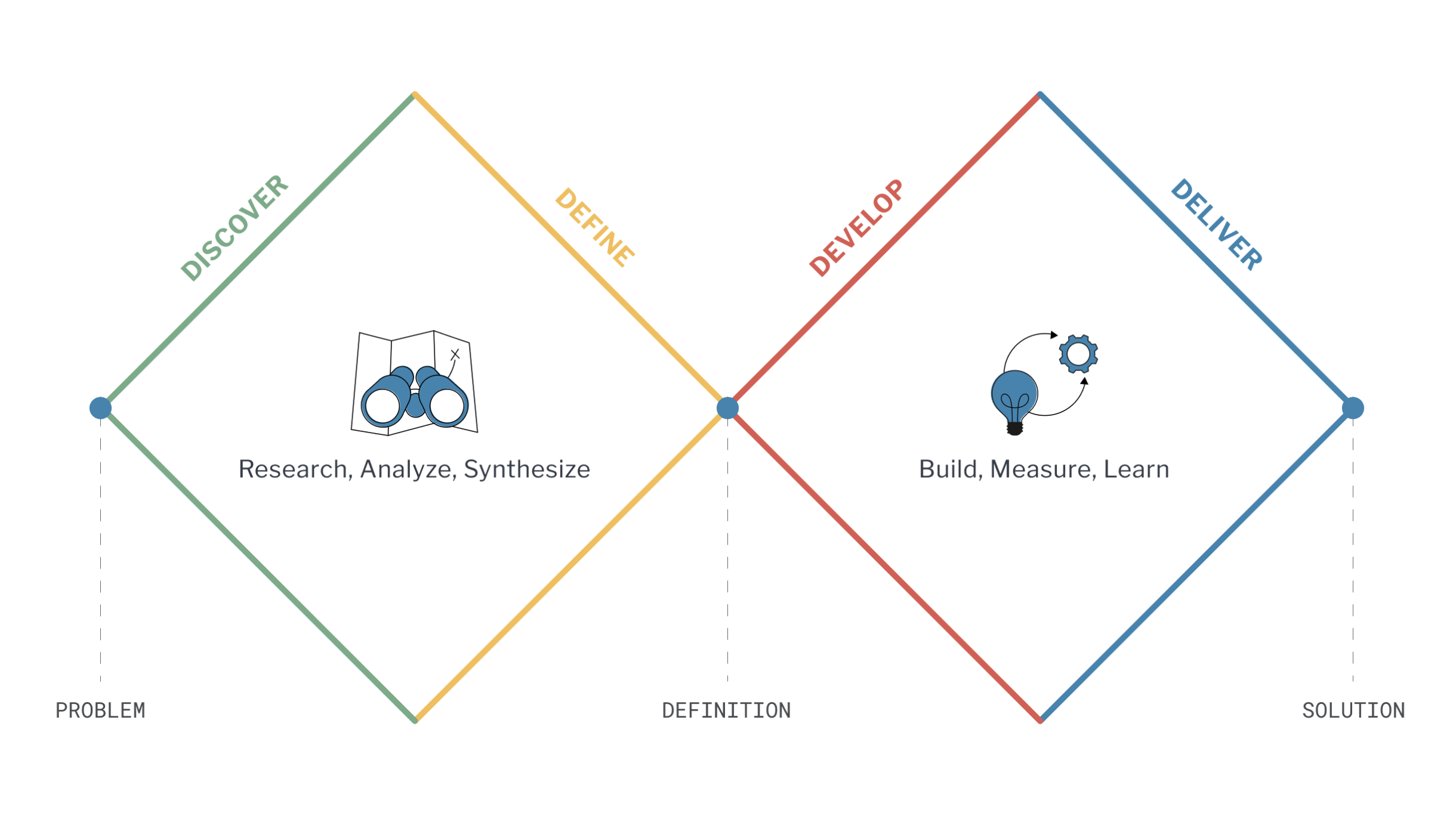
Our team followed an agile, iterative design process that involved four key stages: discovery, problem definition, design and development, and delivery. During the discovery process, we conducted extensive research to understand the challenges and needs of underserved populations regarding HIV testing and reporting, and we then synthesized our research findings to define the problem statement and identify the specific needs and requirements for our solution. Moving into the develop stage, we utilized a range of ideation techniques to generate potential solutions to address the identified challenges, and in the deliver phase, we refined our solution based on user feedback and testing.
Phase 1: Discover and define
Our discovery process included stakeholder interviews with Los Angeles County’s health department as well as other state and local health departments across the U.S., contextual inquiry with community-based testing organizations in LA County, and remote 1:1 interviews with other non-clinical testing providers across the U.S.
Contextual inquiry
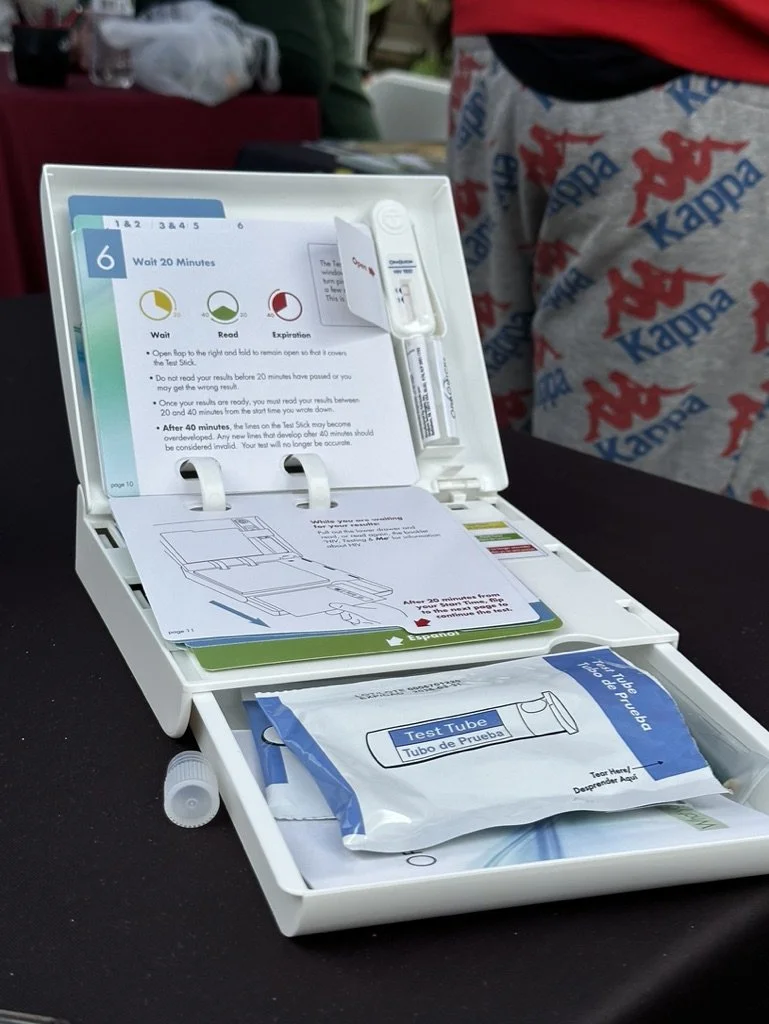
We conducted contextual inquiry with four different organizations conducting HIV and STI tests in Los Angeles County. We immersed ourselves in a number of testing environments, including, indoor drop-in centers, street medicine outreach to encampments, and mobile testing centers. To understand the diverse perspectives and experiences within the community, we conducted six contextual interviews with three different community-based organizations. We spoke with program coordinators, certified HIV testers, health processionals, and case managers, and observed over 30 individuals as they accessed HIV testing services. This firsthand experience provided valuable insights into the testing experience from the perspective of those directly impacted.
Remote interviews
To ensure we could build a solution that addressed the needs of diverse testing settings, we conducted remote 1:1 interviews with 12 HIV testing providers across the country, focusing on non-clinical settings. We developed our interview guides based on insights gleaned from our in-person observations as well as hypotheses formed from our stakeholder interviews.
Analysis
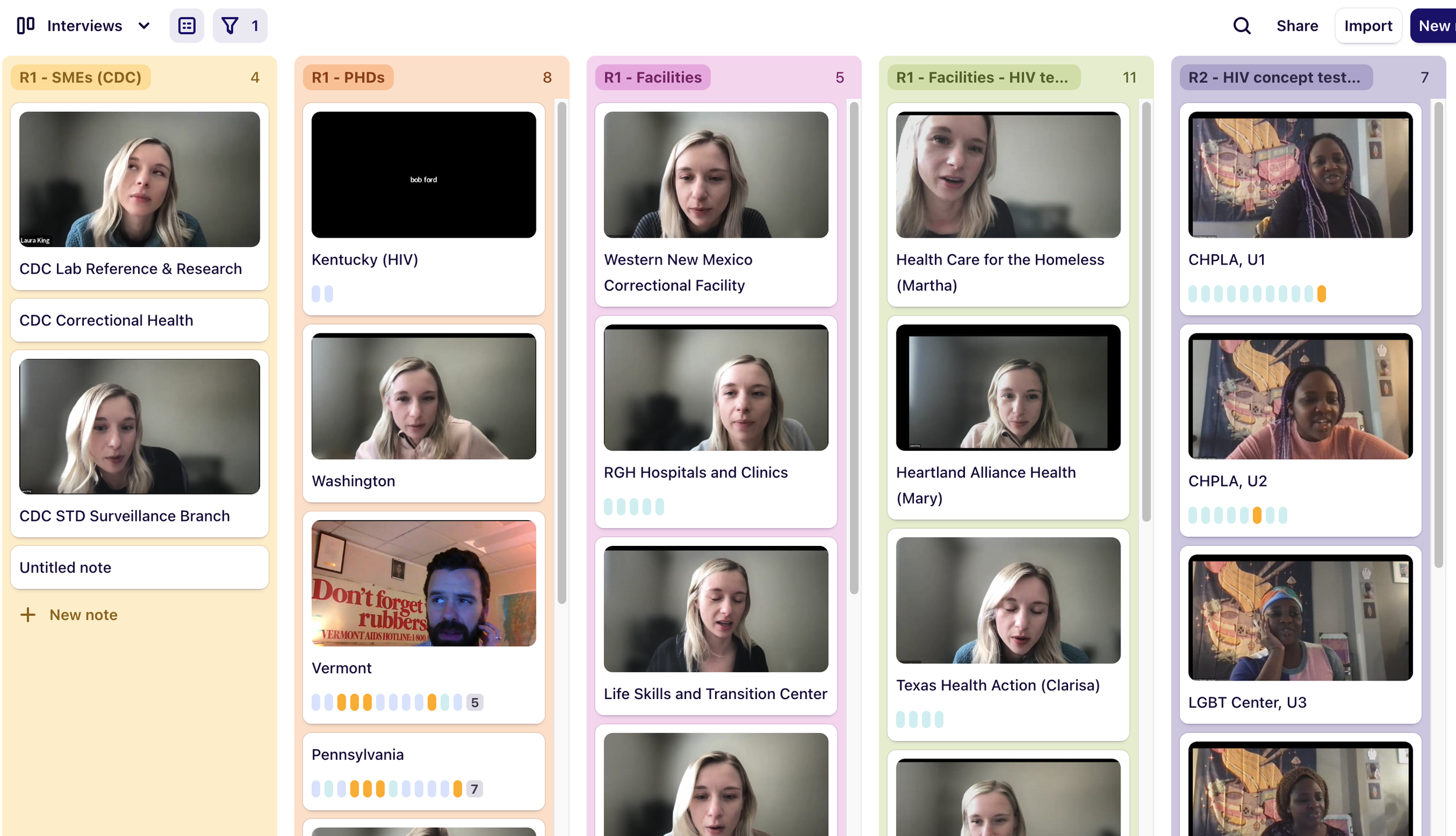
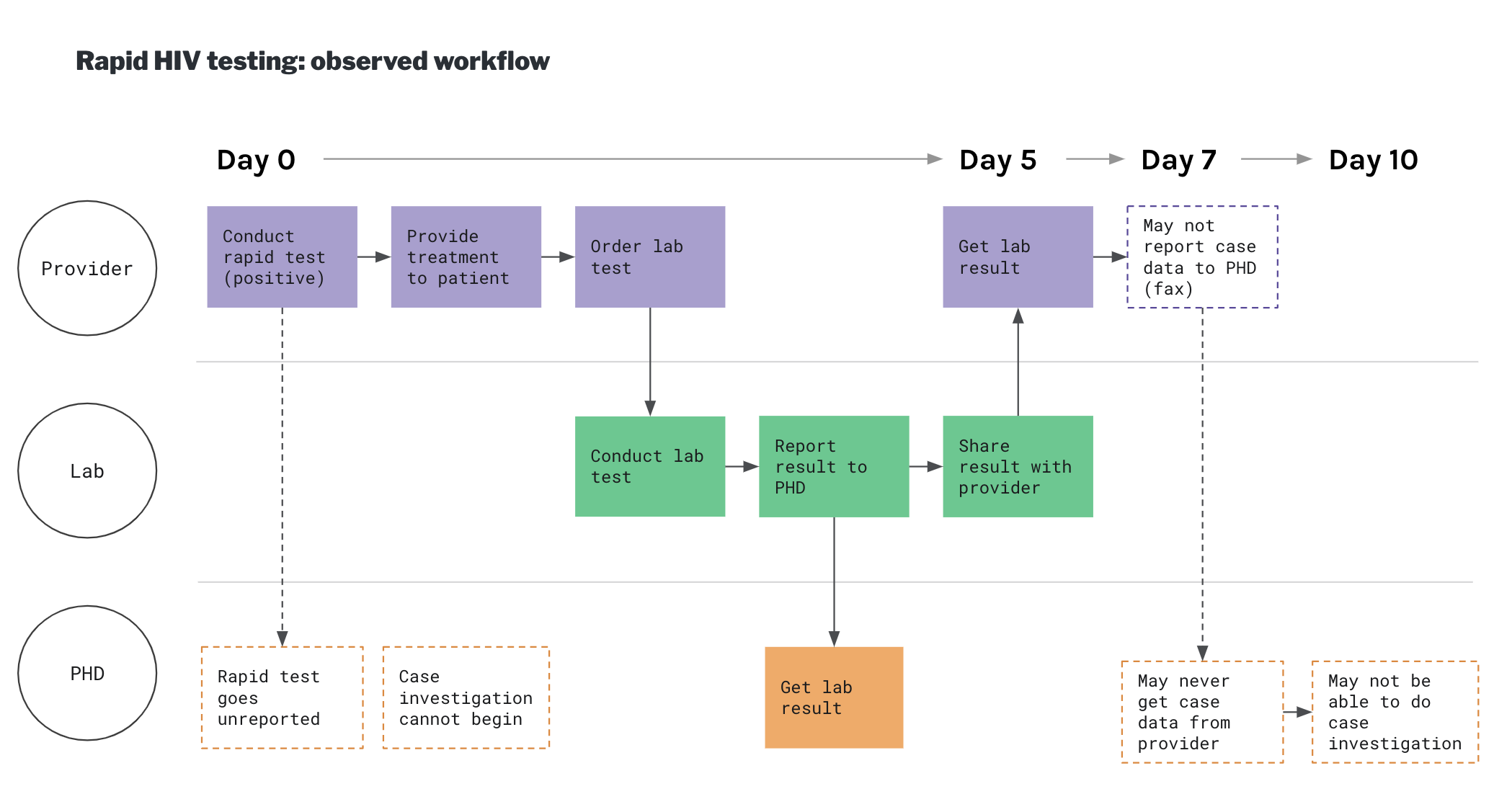
Throughout our discovery process, we held regular debrief sessions as a team where we discussed insights and emerging themes in our research. We also uploaded our observations and interviews to Dovetail and coded our data to rigorously identify recurring themes and pain points in the current process and help our team identify key areas to focus in the develop phase. We developed process maps and diagrams to illustrate testing scenarios and shared our findings through slide decks and other visual artifacts to share back with our team and clients.
Key takeaways from research
The biggest gap in STD and HIV surveillance data comes from missing or delayed case reports from providers, which contain valuable information about patient demographics, symptoms and treatment. The process of reporting case data is very manual and cumbersome, and this information often goes unreported.
Testing organizations rely on lo-fi, manual methods to jot down participant data during testing, transferring notes to digital platforms for reporting later. Testers are often multi-tasking - talking to participants, handing out resources, etc. - all while moving test participants through a queue as quickly as possible.
Protecting testing participant privacy is a priority for testing organizations, and testing participants are often reluctant to share personally identifiable information (which is typically required for public health reporting).
Phase 2: Develop and deliver
Moving into the develop and deliver phase, we explored concepts that would:
Provide a simple, streamlined mobile-friendly interface that supported existing testing workflows
Reduce the amount of PII and/or create options for participants who are unable or unwilling to share PII
Concept testing
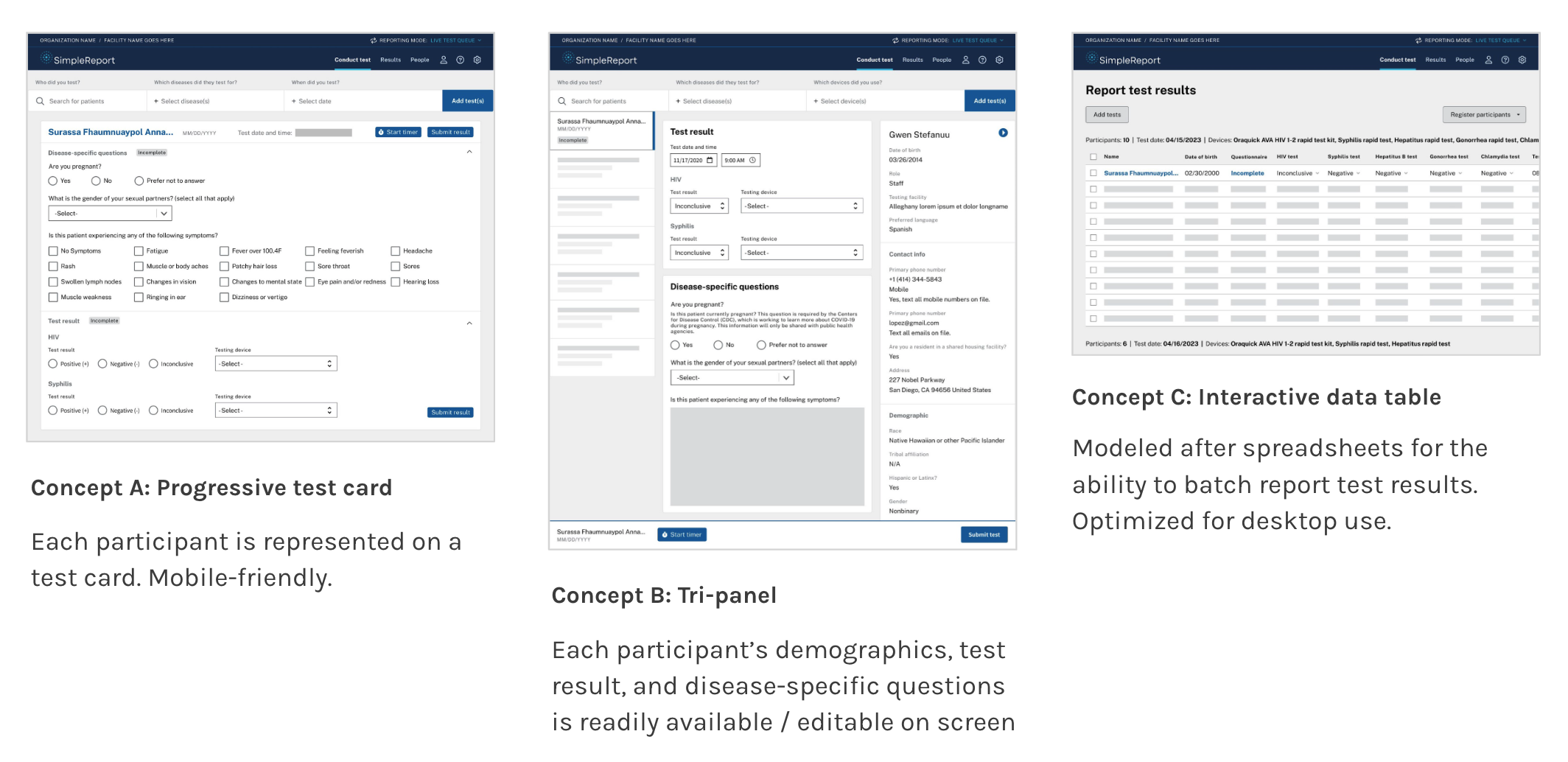
We began our design phase by exploring three divergent concepts to support users’ workflows in a variety of testing environments, and created mid-fidelity Figrma wireframes for each that demonstrated concepts and key functionality. We used these to conduct remote concept tests with 7 HIV testing staff from organizations in LA County and throughout the U.S. The feedback we received helped us identify aspects of each concept that best supported our users’ workflows, and we honed in on features such as progressive disclosure and a mobile-friendly test card design.
Usability testing and iteration
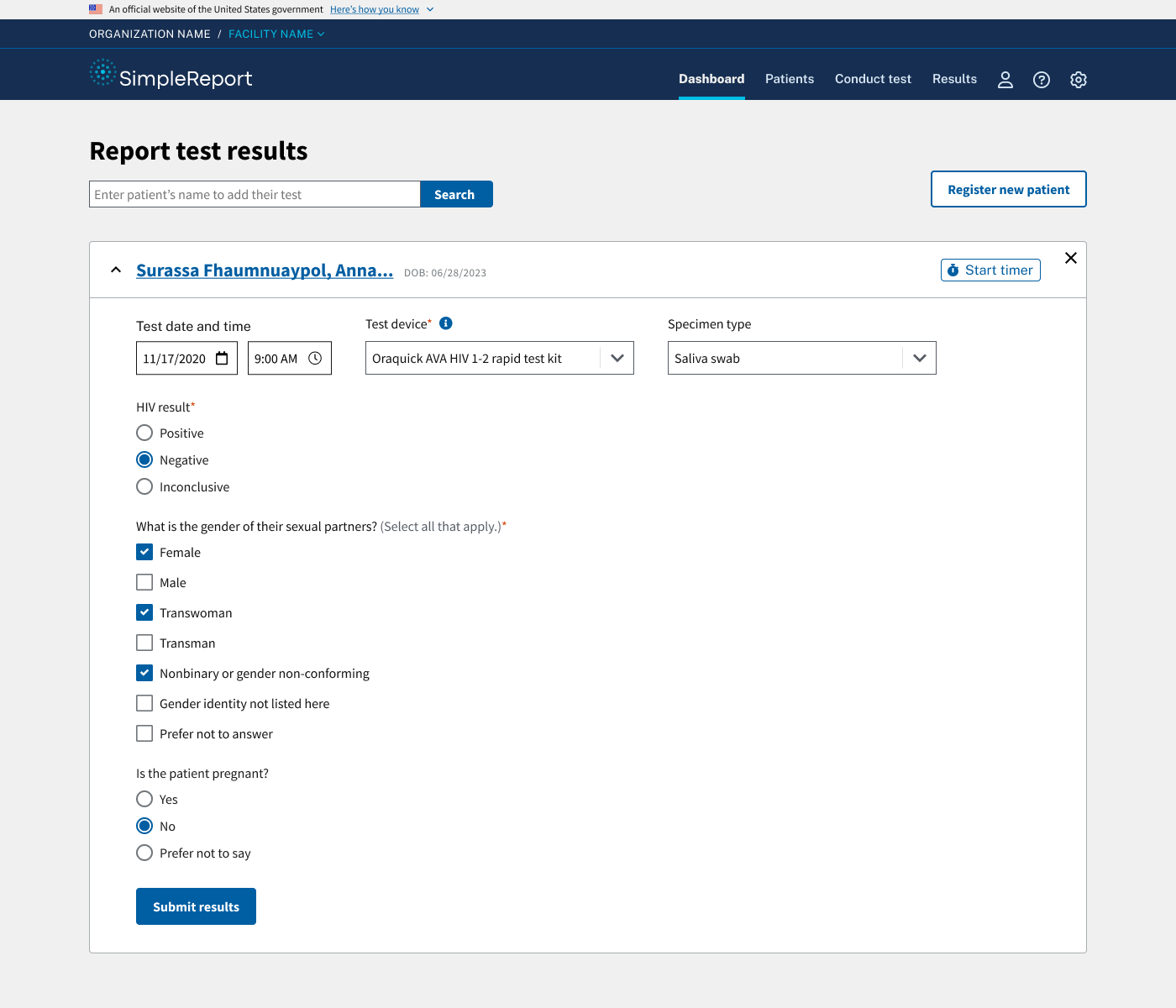
We created more detailed interactions to support HIV testing workflows, building out an interactive, high-fidelity prototype. We then conducted several rounds of usability testing, including 18 remote and in-person sessions with community-based organizations in LA County and users across the U.S. These helped us identify usability issues in the design, along with other features and considerations for successful product adoption. For instance, we learned that we needed additional options to accommodate testing participants who were unhoused or did not wish to share demographic information, so we made changes to our patient registration form to allow users to submit facility information or other notes in lieu of patient address and phone number. We also worked closely with our stakeholders to streamline data requirements, particularly for negative tests.
Implementation and impact
Alongside our research and design efforts, we worked closely with our engineering team to develop a product roadmap and features for an MVP. We launched the HIV testing capability to a closed beta group of testing organizations in Los Angeles County. As users are testing out the tool, they continually praise the ease of use and efficiency, and find the solution supports their testing workflow.
“That was very easy to do - and fast too. I think this will make a lot of testers’ jobs very easy and organized.”
- Beta test participant
Reflections
For this project, we had the challenge of meeting users’ needs that conflicted and challenged with. client constraints. While the CDC and LA County’s health department wanted to collect as much data as possible for HIV cases, we learned that people accessing HIV testing services wanted to share as little demographic data as possible. Testing participants often expressed discomfort with sharing personally identifiable information, citing concerns about privacy and the potential stigma associated with HIV testing, and many participants were unhoused and did not have a fixed address or phone number. By presenting these needs to our stakeholders in a clear and understandable way, we were able to move forward with alignment in designing solutions that managed constraints while providing an excellent user experience.